HIPAA Compliance Software
Achieving and maintaining compliance with the Health Insurance Portability and Accountability Act of 1996 (HIPAA) should be a critical priority for any organization handling medical information. Leverage LogicManager’s HIPAA Compliance software to meet evolving requirements and increase efficiencies along the way.
For additional value:
Why a Risk-Based Approach to HIPAA Compliance is important:
LogicManager’s HIPAA Compliance Software
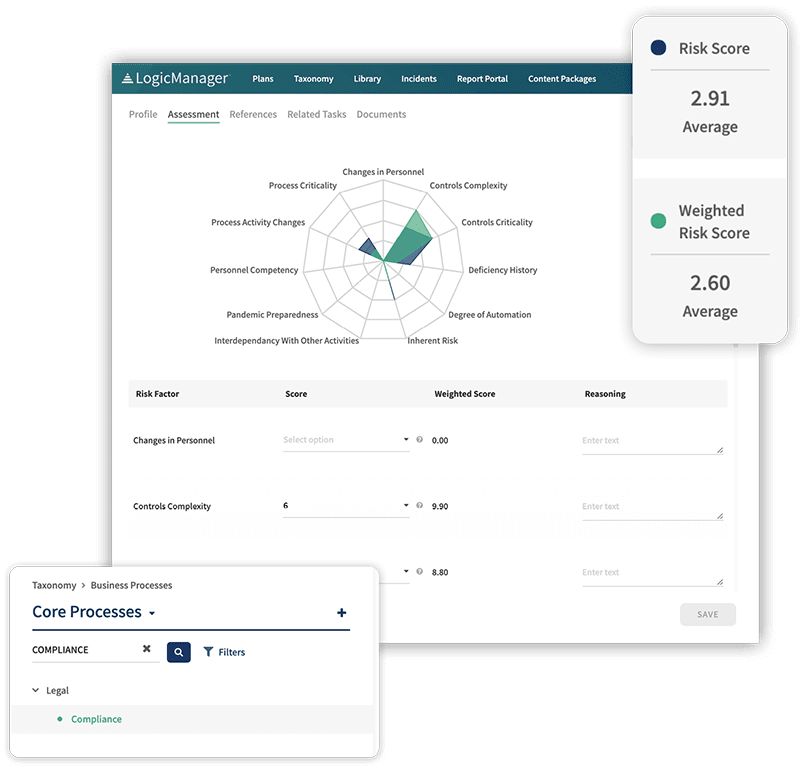
LogicManager’s HIPAA compliance software comes preloaded with:
- Out-of-the-box HIPAA compliance readiness checklists of HIPAA’s Privacy, Security, and Breach Notification Rules.
- Pre-built HIPAA risk assessment templates for Information Security, Data Privacy, and Incident Management, each of which directly align with the three sections of HIPAA.
- A security incident webform to support compliance with the HIPAA Breach Notification Rule by quickly notifying affected parties of a data breach.
- A Centralized Control Library where you can document policies, procedures and controls and link them to your HIPAA compliance checklist to create a clean audit trail, organize your compliance efforts and identify gaps.
- Automated workflows and tasks to help you engage the right personnel in the compliance process with automatic workflows. Assign accountability for each regulatory requirement across the organization, and ensure remediation actions take place following a security event.
- A robust reporting engine that can be used to aggregate your data into intuitive, flexible dashboards perfect for proving compliance and monitoring your compliance status. One example commonly used for HIPAA compliance is our Business Intelligence Report.
- Track annual employee HIPAA certifications by automatically sending out policy attestation tasks. From there, employees can simply upload their most recent certification through a secure webform.
Achieve HIPAA Compliance with LogicManager
 Gain Efficiencies
Gain Efficiencies
LogicManager offers the most efficient approach to meeting HIPAA requirements. Our integrated software enables you to scope, prioritize, track and report on the critical information that’s scattered throughout your organization.
Centralize Your Work
Measuring and achieving HIPAA compliance is a large undertaking without comprehensive software, as using various applications to cover the scope of it is time consuming and allows room for error. With LogicManager, every tool you need to achieve compliance is centralized in one intuitive platform.
Achieve Compliance Quickly
LogicManager is a SaaS solution, which enables us to deploy customer environments virtually and efficiently. Because of this, our customers are up and running in the system within 5 business days.
What is HIPAA Compliance?
Healthcare recordkeeping is moving full speed ahead, and will soon be entirely paperless. Few hospitals and insurance offices still keep hard copies of patient files safely guarded behind lock and key. The shift to electronic health records (EHR) has brought many benefits: greater efficiency, wider access, and seamless communication between practitioners and provider networks. However, by putting information (once only exposed to physical threats such as break-ins or fires) in digital format, we open an entirely new realm of threats that must be mitigated. Faulty hardware, insufficient authentication, inadequate backups, and unintentional disclosures are now pervasive threats across all healthcare and service providers.
The Health Insurance Portability and Accountability Act of 1996 (HIPAA) is U.S. legislation that provides data privacy and security provisions for safeguarding medical information. HIPAA applies to any entity that takes healthcare insurance and any entity that provides healthcare services. The main purpose of HIPAA is to standardize the tracking and security of electronic healthcare transactions. HIPAA compliance requires organizations to implement safeguards that protect the confidentiality, integrity, and availability of electronic protected health information (ePHI).
HIPAA Risks
What can happen to your organization if you fall short in complying with HIPAA? The repercussions could be catastrophic, with potential legal battles and regulatory fees. Additionally, the potential for reputational damage if you’re found to be fraudulent or noncompliant could mean the end of your organization entirely. The penalties for HIPAA noncompliance are based on the perceived level of negligence, and can range from $100 to $50,000 per individual violation, with a max penalty of $1.5 million per calendar year for violations. Violations can also result in jail time for the individuals responsible.
Related HIPAA Content
Request a DemoLearn How LogicManager’s HIPAA Compliance Software Can Transform Your Risk Management Program
Speak with one of our risk specialists today and discover how you can empower your organization to uphold their reputation, anticipate what’s ahead, and improve business performance through strong governance.

 Gain Efficiencies
Gain Efficiencies

